Dr Liz Mear
Explaining Connected
Health Cities

Connected Health Cities (CHC) was a £20m, four-year pilot funded by the Department of Health to unite local health data and technology to improve care for patients in the North of England.
The North has some of the worst health outcomes and a vast and widening gap in healthy life expectancy compared to the rest of the UK.
CHC recognised there was potential to close this gap by connecting information held by the NHS and social care to plan and deliver systems more effectively.
Co-ordinated by the Northern Health Science Alliance, the ground-breaking project linked academics, clinicians, people and industry to create a Learning Health System and put patients at the heart of how their health data was used whilst supporting local industry and boosting the region’s economy.
The programme was delivered in four regions:
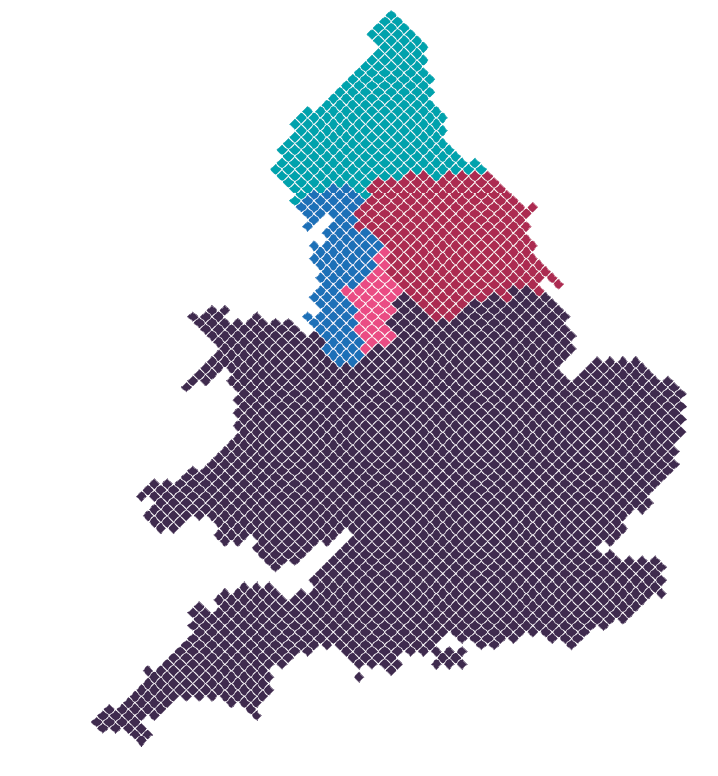
- North East and North Cumbria
- Yorkshire and Humber
- Greater Manchester
- North West Coast
In four years, Connected Health Cities delivered outstanding results:
What has been achieved is now reproducible and the CHC methodology is being shared with other UK health programmes
Connected Health Cities in the North West Coast
The North West Coast CHC harnessed the power of data to improve care for patients with Chronic Obstructive Pulmonary Disorder, alcohol-related liver disease and epilepsy.
These conditions pose a real challenge to health and care systems in the NWC which covers Cheshire, Merseyside, Lancashire and South Cumbria and has 4.1 million residents.
The NWC CHC looked at ways that data can be used to support clinical teams to improve the care pathways for patients with these conditions.
The programme was delivered by Health Innovation North West Coast in collaboration with the University of Liverpool, Lancaster University and AIMES Management Services.
The partners developed a ‘Learning Health System’ which involved collecting, linking and analysing data from health and social care and presenting information to frontline staff to help them to plan and deliver care more effectively creating a continuous cycle of improvement.
The CHC methodology is now transferable to other chronic conditions and we have developed a ‘toolkit’ to share with local health systems.
Julia Reynolds, Associate Director for CHC, said: “We will be building on this important work in the future and spreading our learning to other pathways.”
To find out more visit www.chc-impact-report.co.uk
Continue reading: The Clinical Pathways >